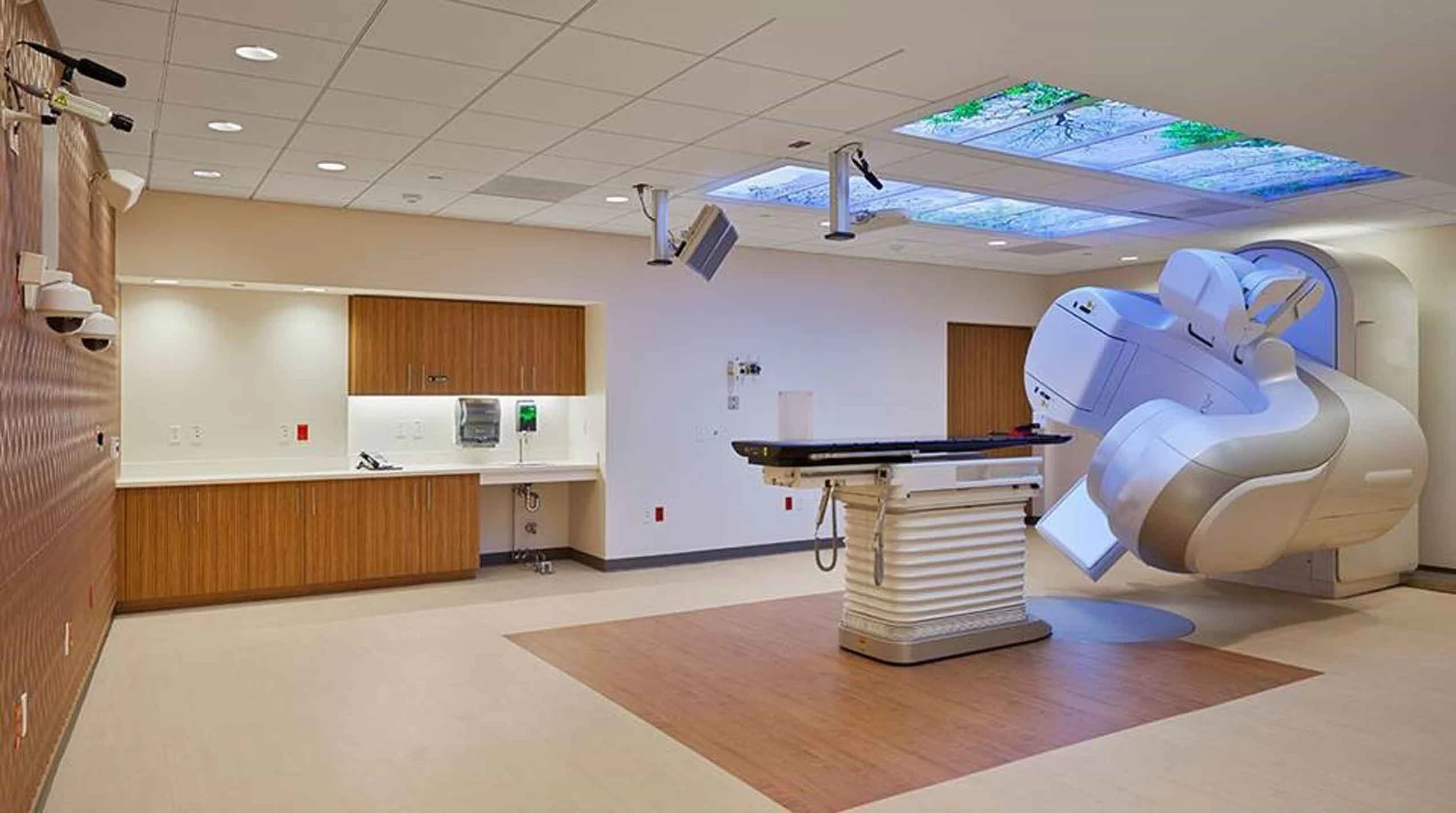
Designing the New-age Oncology Radiation Therapy Department
By Nandini Bazaz
Hosmac’s Ar. Nandini Bazaz elaborates on designing an efficient, functional and patient-centric radiation therapy (RT) unit.
‘Sorry, we have detected a tumour in your…,” informs the doctor.
A common news for patients and doctors, considering 17 million people are detected with cancer every year. This diagnosis can be devastating for anyone. Not always a death sentence today but living with cancer can be terrifying, regardless. It is imperative to treat cancer patients with compassion and empathy, not only by doctors and nurses; what if we could incorporate these very qualities in cancer facilities? The answer lies in building them by keeping cancer patients at the heart of the design. This article will deal with designing a radiation unit for patients needing radiotherapy.
What is Radiation Therapy?
Radiation Therapy (RT) is a clinical specialty division for treatment of cancer through radioactive rays generated in a medical equipment by the name of Linear Accelerator (LINAC). The radiation treatment is planned to damage the cancer cells barring the healthy cells by planning concentrated treatment to the most specific tumour cells through external beam therapy. It is a malignant tissue-destroying procedure, carefully planned by a highly trained medical team comprising oncologists, medical physicists and technicians.
High-energy particles (waves), such as x-rays, gamma rays, electron beams, or protons, to destroy or damage cancer cells are accelerated in the LINAC machine at time of transmission and is present in the bunker.
In most cases of cancer, radiation therapy is the first line of treatment, though can be coupled with Chemotherapy which exposes the entire body to cancer-fighting drugs, whereas radiation therapy is usually a local treatment.
Departmental Location
Locating the bunker in the ground level next to Diagnostic Imaging department is okay if space permits. Especially for flood-prone sites, for example parts of Kerala, Mumbai, Chennai and a rocky terrain too, as there exists high cost of piling, locating the bunkers on ground level may at times be the preferred option.
In levelled land plots or plains, constructing the RT department in basements can be opted for too. For basement bunkers, a hatch in the road should be planned in advance to lower the LINAC equipment from ground level; and the entire RT department should be developed on that same level of basement preferably. Yet, in both cases, whether on ground or in the basement, route of rigging (path) of radiotherapy equipment should be planned keeping in mind the traverse of this 8.5 ton (approx.) equipment.
Bunkers are mandated to conform to BARC shielding requirements. Ideally, the bunkers are planned in 2.4 meters thick walls and ceilings of concrete. High density materials (like, concrete or steel) should be used in walls, ceiling and floor. AERB permissions are required. Floor loading should be planned with respect to equipment loading.
Departmental Zoning
To begin with, map the sequence of patient movement in the facility. It usually follows a traditional path. Hence, a zonal design facilitates a more relaxed navigation.
A radiotherapy unit can be divided into a few transitional zones:
Public zone comprises a reception area (the control station) and a waiting area for family members (after patient is taken into patient zone)
Patient zone consists of a changing room for patient and a waiting area for the patient before he/she is taken into treatment zone.
Treatment zone is the area where patient receives radiotherapy. It consists of LINAC or Linear Accelerator bunkers, Brachytherapy, console/control room (occupied by oncologists and technicians). LINAC is the equipment present in the bunker to eradicate cancer cells.
Treatment Planning zone is where doctors sit (preferably in seclusion) to plan the radiotherapy procedure. It consists of consultation/doctor rooms close to a mould room. Customized mould helps to hold the patient in the right position and restrict movement during radiotherapy.
The LINAC department also carries with it a CT simulator and a PET/CT simulator for enabling radiation oncologists to use multiple imaging techniques by localizing and targeting the tumor with high-tech precision to enhance the accuracy of radiation treatment planning.
Care Provider zone is where the medical personnel work from to attend to the patients. Also, caregivers should preferably have the ability to see the patient and have accessible supplies/equipment.
Equipment/Units
Cobalt unit is used for deep radiation therapy.
In the LINAC, the electron beam is typically created as cancer-killing radiation to tumors of varying size and shape, sparing surrounding healthy tissue. Using a high-energy electron (particle) beam accelerator, i.e. the LINAC, the medical team is able to kill a patient's malignant cancer cells.
CT Simulator is utilized to set telegraphy field and plan radiation treatment. Simulation is the process with which the radiation oncologists, physicians acquire images of the body in order to develop the appropriate treatment plan.
Brachytherapy is a method of delivering radiation to tumors where radioactive sources are placed either within or immediately adjacent to tumor tissue.
Functional Programming
The functional program of a clinical department describes the requirements which it must satisfy in order to support and enhance the activities of the services in the clinical unit. Detailed programming is developed by clinical program recommendations by users; be it doctors, staff, patients, care-givers and in some cases even educators/researchers. Through staffing indices one is able to derive the staff numbers and utility zone capacities. Data on the type of equipment to be planned and standard layouts for specific needs will allow factoring in the usage of such areas. The functional programming document then leads us to space requirements to plan the department to accommodate clinical as well as non-clinical areas, parts of horizontal and vertical circulation, as well as additional built-up areas included in the gross departmental area.
Layout
Radiation Therapy commonly maintains two patient care areas; treatment planning (mould room) and radiation treatment (LINAC bunkers). Treatment planning with assessment and evaluation generally occurs during the patient’s initial visit. After a treatment approach is determined, the patient generally accesses the treatment area repeatedly during the course of treatment.
Space Programming
Radiation Oncology
Regulatory – AERB (BARC) Certification Process
Clearance certification from RT unit by AERB
Approval of room layout plan (1:50 scale)
Construction can start only on basis of approved plan
Any modification shall be re-approved
Appointment of staff
Nomination and approval of radiological safety officer
Construction & Shielding Materials
The LINAC bunker is built with concrete that has a density of 2.35 g/cm3. Around the world, especially in the West, steel is also used as the shielding material of choice;
however, its construction works out to be over as high as seven times the price of concrete bunkers. Concrete is the least expensive material in this regard and hence commonly used. As space can be a constraint, a material with greater density can be used.
Shielding material densities in gm/cm3:
Earth is 1.6
Concrete is 2.35 (cheaper works, thickness more)
Heavy concrete > 2.35
Steel is 7.9
Lead (Pb) is 11.35
Approach to Design
Patient: A patient, when he/she comes in, will require social support. For same, when accompanied by relatives, an isolated and quiet zone to receive him/her is preferred, away from large gatherings of people coming into the healthcare facility. Aim is to create an ambience of calm, peace rather than commotion. Likewise so, areas where one can view nature, or look out into areas harnessing daylight, or even shaded sunlit environments, greatly enhance the dim mood a patient might be experiencing, thus enabling hope. As mentioned earlier, privacy of movement and seating (waiting) to such patients is also a factor of mindful design achievement which aims to shield them off from experiencing discomforts and/or anxieties they might be undergoing in course of the treatments.
For quick action by staff, nurses and technicians, quick visibility to patient zones is a plus. Likewise so, floor control with respect to places for family and guests also comes under staff observation. Overall, tranquil, comfortable, modern environment, which can male possible experiencing peace and serenity becomes key to a successful design strategy for the RT department.
Staff: While planning for staff in the RT department, it should be kept in mind that they ought to reach the key areas through minimum walking distance. As stated earlier, patient visibility enhances staff reach to patients in case of emergency as well as steering of patients for treatment sequentially.
At the same time, collaboration with nurses and other staff also becomes easier when emphasis on carefully planned reach-out-routing is implemented; including easy access to supplies (reduction in walk path).
It is also advised to plan spaces for private conversations and resting for staff with ease-of-access to washrooms. As staff will be spending a lot of time in and around the LINAC, CT SIM and Brachytherapy spaces, which is a lot of equipment, and practically no connection to outdoors, it is then advisable to design refreshing breakout spaces for respite and to create supportive environments for the caretaker team. To complete the whole, realization of ergonomic studies greatly benefits suitable design and planning of staff needs and services' routes.
Physicians: A physician's convenience is supreme, hence their movement in the RT department is primarily to be assessed in terms of their reach to treatment and planning rooms, from his/her office. In the same line of thought, efficiency to reach nurses and staff should also be accounted for. Yet, in the entire gamut of allotment of spaces, the doctor is to be handed over areas where he can maintain privacy, comfort, and also an area for rest.
A physician should also have his area planned to enable access to advanced technology as information received and exchanged by various other teams (oncologists, doctors, technicians, therapists) is key to the treatment planning process.
Medical Equipment and Technology: The medical equipment like LINAC, CT SIM, Brachytherapy machine ought to be the latest, most effective, smallest, lightest and fastest. With competition driving the healthcare segment, it is advisable to keep abreast with latest technology in medical equipment as the investment by the stakeholders is high.
The machines have to be comprehensive and user-friendly, at the same time. Adaptability as well as flexibility are two other factors which enable precise treatment and better quality output in cancer cases.
Administration/ Executive Leadership: The heads of departments and administrators are the ones who inspire the department to run without glitches by ensuring productivity is maintained, ease of service is provided and smooth work flow is practiced. This is implementable by effective operation processes and systems which are conducive to the useful functioning of the department.
As these are revenue generating departments and spaces, care is to be taken for overall efficiency is sustained for prolific outcomes.
Architecture: One of the most important influences of a medical department is its architecture. Spaces which are being planned for handling emotions of a person must be sensitive to people inhabiting the hospital, short term or long duration, either way. Interior design spaces are to be intended for ease, calm, peace, comfort, assurance and uplifting of the senses.
At the same time, these must be appropriate in image and cost; rightly suiting the context (patient, religious sentiments if any) of the society and/or the stakeholders. Even the comfortable aspects applicable to doctors, staff, nurses, technicians, who visit the hospital for the services must be included in developing the language of the architecture of such spaces.
A good practice is to amalgamate ecology and environment as improved healing effects of the natural surroundings is a definite upshot.
In a Nutshell
RT department is planned keeping in mind many factors which might influence its location as the weight of the concrete bunkers will limit the location of this facility. By ascertaining its location with respect to site factors, project's existing structures, and also an analysis of surroundings will enable the designer to narrow down its location.
RT Department is primarily a standalone facility however it can be amalgamated with other clinical departments in the vicinity, preferably of the same discipline like Nuclear Medicine or Chemotherapy department and/or also the imaging department commonly known as radiology also; to share staff and spaces with these allied systems.
It will be necessary to be understood, earlier in the design and planning of a department, that proper functional adjacencies will enable operational efficiencies; amongst staff and patient. One will also be required to plan to allow adaptability and flexibility in technology as regards to medical equipment and information technology.
An outpatient coming to this facility, is often weak, stressed and anxious, not knowing how the illness has gripped him/her. Hence, patient privacy, poise and decorum are to be considered as principal parameters of staff responses to such patients; infused with serene interior design concepts in the RT departmental planning. Way-finding will need to be clear enabling easy access routes to these outpatients who are in need of a stress-free environment.
Some interior spaces planned for the RT department should be designed keeping in mind possibility of access to natural light; inclusion of sights and sounds of nature; creating indoor gardens; pleasant artwork in corridors can be put up; wood-work to be used to create a warm effect and also plan family-friendly facilities. These styles will enable anxiety-prone patients and their families to experience calm assuring sentiments, thus better optimistic outlooks can work well for patients and families. Positive distractions can be created by installing pleasant imagery on the walls or ceilings, especially in treatment rooms like the LINAC gantry, CT SIM room, Brachytherapy area, that can help a patient to alleviate stress or anxiety whether seated or in supine position. Apart from the illness itself, the strain is due to complexity of the procedure/s, besides the intimidating equipment which is handling the procedure. All this requires sensitive analysis and thus, careful delivery of reassuring, encouraging interior spaces will go a long way.
Author
Ar. Nandini Bazaz
Ms. Nandini Bazaz’s has worked extensively on various multi-specialty hospital projects. She has designed 20,00,000 sq ft of space and has played managerial roles in Space Programming, Facility Planning, Architectural Design and Design Consultancy work for many healthcare facilities. Ms. Bazaz is a member with Council of Architecture and is certified by Canadian Architectural Certification Board (CACB).