Ayushman Bharat: What has changed in the Healthcare Sector a year on?
September 23, 2019, marked the completion of PM-JAY's first year. PM Narendra Modi had launched PMJAY on September 23 2018, from Ranchi, Jharkhand. Healthcare Executive looks at the key milestones of the scheme.
During the year gone by, National Health Agency has covered substantial ground. 10.3 crore e-cards have been issued to beneficiaries and treatment amounting to Rs. 7,490 crore was pre-authorised in different parts of the country. Every second, three e-cards are being distributed, and every day, 51 hospitals are joining the network, which brings healthcare to PM-JAY beneficiaries. [1] PMJAY has been rolled out for the bottom 40 per cent of a weak and vulnerable population. In absolute numbers, this is close to 10.74 crore households.
Vision of PMJAY
The Vision of PMJAY for the next five years is to accomplish SDG 3.8: Guaranteeing financial security against catastrophic health expenditure and access to affordable and quality healthcare for all.
Facts
As on September 22 2019, 32 states and Union Territories are executing the scheme. A total of 10.3 crore e-cards have been dispensed. Further, 46.5 lakh hospital treatments have been completed. The value of treatments provided is close to Rs 7,490 crore. Also, 18, 236 hospitals have been empanelled. According to authorities, 45 lakh calls have been answered by NHA Call Centre (14555). There are 1.5 crore users on mera.pmjay.gov.in and 3.8 lakh PMJAY app installations.
Implementation Models in States/UTs
The various States are using different models for implementing their own health insurance/assurance schemes. Some of them are using the services of insurance companies, while others are directly applying the schemes in their States.
Because States are at different levels of preparedness and have varying capacity to manage such schemes, PM-JAY provides the States with the flexibility to choose their implementation model. They can implement the programme through an assurance/trust model, the insurance model or a mixed model.
Partnerships
NHA has also entered into alliances with several governments, non-government, multi-lateral and not-for-profit organisations. The goal is to synergise knowledge and skills to make the implementation of PMJAY more effective.
Some of them are German Government, the World Bank, Bill and Melinda Gates Foundation, International Innovation Corps, Clinton Health Access Initiative, Asian Development Bank, National Skill Development Corporation, Department of Health Research, National Cancer Grid, Quality Council of India, ICICI Foundation for Inclusive Growth, Common Service Centres, Nathealth, Wish Foundation, PHFI and Insurance Institute of India.
Progress Report
Beneficiary Identification Process (BIS) helps verify beneficiaries from the entitled database, and build an authenticated beneficiary registry. The BIS is one of the components of NHA's information technology backbone. It allows for combing beneficiaries through SECC or additional datasets through Application Programme Interface (APIs) and supports Aadhaar eKYC (electronic Know Your Customer) and non-Aadhaar based KYC for authentication.
Creation of Hospital Network
To cater to the increased requirements under PM-JAY and to secure quality care to the beneficiaries, it is crucial to sustain and expand a network of hospitals that also adhere to the quality standards and criteria. This leads to the demand of empanelment of hospitals on a pre-emptive basis so that recipients are confident of their rights being honoured in the most convenient, cashless and quality manner.
Empanelment Criteria
Agencies have devised two types of empanelment criteria— general criteria and unique criteria for clinical specialities. It is based on supply-side characteristics (nearly 71 percent of the hospitals are running as proprietorship businesses with less than 25 beds capacity and offering non-specialised general clinical care). These guidelines have been changed based on the experience of the accepted practice in other Government-funded health insurance schemes, State-specific statutes related to the quality of care and Clinical Establishment Act 2011. The detailed guidelines for empanelment are available on www.pmjay.gov.in.
PMJAY prescribes a two-tier approach to the empanelment of hospitals, which is online, lucid and practical, and is free for all steps of the process. A hospital can be empanelled by the district empanelment committee or by the state empanelment committee. The state has the final decision making power.
Statistics related to hospital empanelment and hospital admissions are summarised below: (as on September 22, 2019)
Although States are in charge of the empanelment of hospitals, there are renowned tertiary care hospitals and specialised care hospitals that operate as autonomous institutes of excellence directly under the MoHFW or some other department. Most popular examples of such hospitals are AIIMS, Safdarjung Hospital, JIPMER and PGI Chandigarh. The NHA has empanelled these hospitals directly by signing an MoU with each of the facilities. Also, all NABH accredited private hospitals in the National Capital Region (NCR) are directly empanelled by NHA to widen the network of service providers.
Health Benefit Packages
PM-JAY has 1,393 treatment packages out of which 1,083 are surgical, 309 medical and one unspecified package.
Beneficiary Awareness
The National Helpline – 14555/1800 111 565 was set up by the National Health Agency on August 24 2018.
Source: PMJAY Annual Report
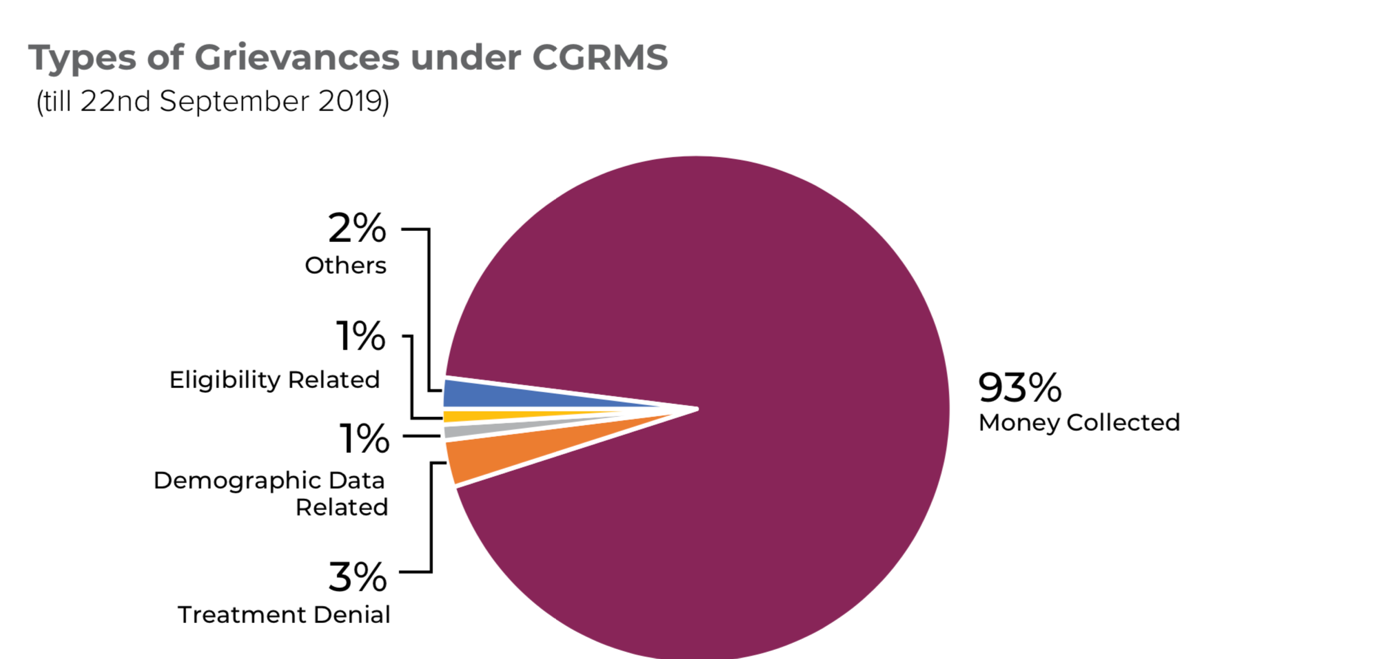
Grievance Redressal
A three-tier Grievance Redressal Committee structure has been set up at National, State and District levels for this purpose. These committees track and monitor the grievances and its status, collect additional information from parties involved, facilitate hearings, review records, adjudicate and issue orders on the complaint and ensure compliance of committee orders. The Central Grievance Redressal Management System (CGRMS) is an online web-enabled system developed to redress PM-JAY related grievances. The CGRMS primarily aims to enable submission of claims by the aggrieved party from anywhere and anytime (24x7). Steps were taken to revamp the existing portal to make it more user-friendly.
Source: PMJAY Annual Report
Fraud Prevention, Detection and Control
The National Anti-Fraud Unit (NAFU) has been set up by NHA for implementing a framework, and monitoring performance with the support of State Anti-Fraud Units (SAFUs) created at the State level. The critical tasks carried out by NAFU relate to capacity building, the launch of Proof of Concept (POC) project for data analytics and commencing medical audits in States. It has also issued Anti-Fraud Advisory Notes for operational level actions to be taken by States in different areas, like the beneficiary identification system, hospital monitoring, and action against fraudulent entities.
Source: PMJAY Annual Report
Speeding in to the Future with PMJAY
In the coming months, the following additional actions are planned,
Advanced analytics with predictive modelling and risk scoring of entities
Integration of Artificial Intelligence layer with real-time alerts to concerned stakeholder
Anti-fraud public messaging
Name and Shame guidelines
Strengthening of legal provisions to effectively deal with fraudsters .
Delivering a developmental programme to people is not a simple affair. For a national programme, it frequently involves a workforce of thousands and a clientele of tens, of millions. It also requires anticipating abuse and plugging gaps through which unscrupulous elements can exploit the system. The field of implementation is also changing fast with quick adoption of IT and the internet by the government. E-governance is visualized to be a game changer for public service delivery. And is proven by PMJAY.